At first glance, Laurie Soffiati may not appear to have the resume of someone tapped to play a key role at a French AI healthtech startup that has been thrown into the global spotlight.
A graduate of France’s elite public administration school, ENA, and former head of digital health at France’s national healthcare system, l'Assurance Maladie, she has a background on paper that screams establishment and insider. Certainly, it's not the profile of someone preparing to join the wave of companies trying to disrupt the system.
And yet, after three years evaluating digital health tools from inside, she came to a blunt conclusion:
“Many of the health tech products I saw were not actually that effective.”
And so, in January, she left behind the life of a French civil servant to become Managing Director of France for Nabla, the Paris-based startup that has developed an AI assistant for clinicians that automates documentation, coding, and EHR workflows in real time, evolving into an adaptive, agentic platform that supports care delivery across settings. Soffiati is betting that AI is now finally ready to deliver on healthtech’s long-standing promises.
While she may be taking on this challenge at a pivotal moment in the evolution of AI, she is also joining the company just as it garnered international attention thanks to its association with AMI Labs, the Paris-based world models startup that recently raised a €890B Seed Round. Through partnerships, founders, and funding, the two companies share an unusually close pedigree, which has given Nabla's profile a sudden boost, with all the recognition and scrutiny that comes with it.
A front-row seat to what doesn’t work
Soffiati’s trajectory is unusually operational for a senior civil servant.
During the Covid-19 pandemic, she was deployed to the Alpes-Maritimes prefecture, overseeing vaccine logistics across a complex, mountainous region. “We had to ensure people didn’t have to drive too far to get vaccinated,” she recalled.
She later joined Assurance Maladie in October 2022 to build its digital health and telemedicine team, placing her at the center of efforts to modernize the nation's national healthcare system.
The new department was tasked with spotting promising tools, evaluating their impact, and helping define how they should be regulated and reimbursed. The goal was simple but ambitious: make sure innovation actually improves care, rather than complicating it. In practice, that meant turning a fragmented wave of apps and services into something more structured, effective, and aligned with public health priorities.
That role gave her something rare: a true filtering position to sort through a fast-moving ecosystem and judge what delivered value and what did not. During those three years spent assessing which healthtech tools could realistically be integrated into the system for reimbursement and which could not, she often saw underwhelming results.
“Many solutions were built as pure tech products first, without doctors,” she said. “And many were at a very early stage and not actually that effective.”
She also noticed a recurring blind spot among startups. Faced with limited funding, many assumed the public system would eventually foot the bill.
“Assurance Maladie is not there to finance innovation," she said. "Its role is to reimburse it once we know a product actually works.”
Good intentions, in other words, are not enough. Clinical value has to be proven.
A breakthrough solution addressing a real health pain
It was in that context that Soffiati first encountered Nabla. At the time, AI medical assistants were emerging fast, but the space was fragmented and noisy.
Her question was simple: “Does it really save time?”
Time is one of the real currencies of healthcare. Doctors are estimated to spend up to 40% of their time on administrative work such as writing notes, filling forms, and updating records. These are tasks that take time away from patient interaction.
In that respect, Nabla stood out immediately.
“I saw the product work, and I was pretty amazed,” Saffioti said.
Nabla was founded in 2018 in Paris by Alexandre Lebrun, Martin Raison, and Delphine Groll, three repeat entrepreneurs and AI engineers, including former Meta/Facebook AI researchers who had previously built and sold startups in conversational AI. The company was born out of a desire to apply cutting-edge AI to something more meaningful than advertising, with the founders even launching their own digital clinic early on to better understand clinicians’ day-to-day workflows.
Since then, Nabla has steadily scaled alongside the rise of generative AI in healthcare, positioning itself as a leading “ambient AI” assistant for clinicians. The company has raised around $120 million in total funding, including a $70 million Series C in 2025, as it expanded from note-taking into broader clinical and administrative automation.
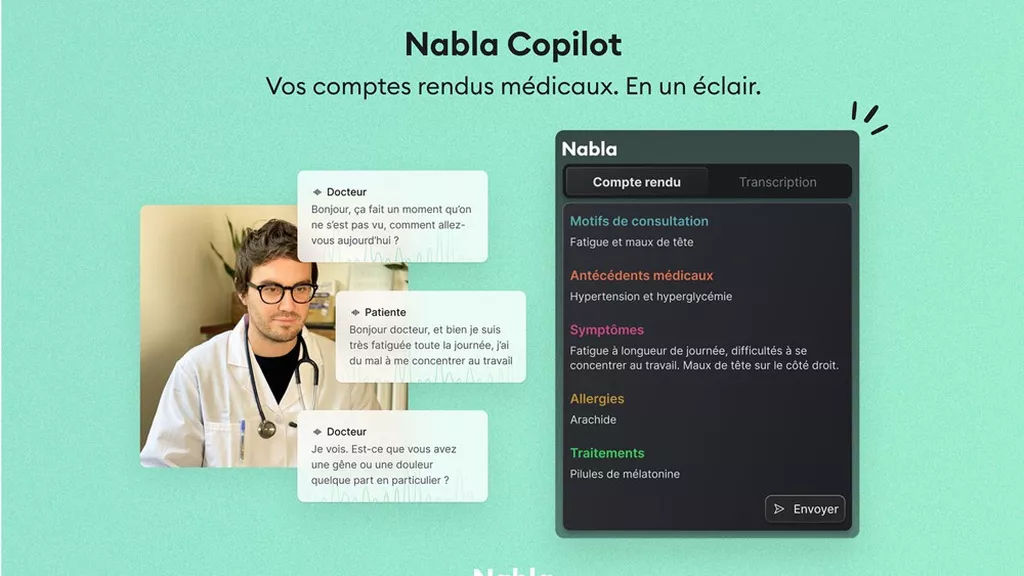
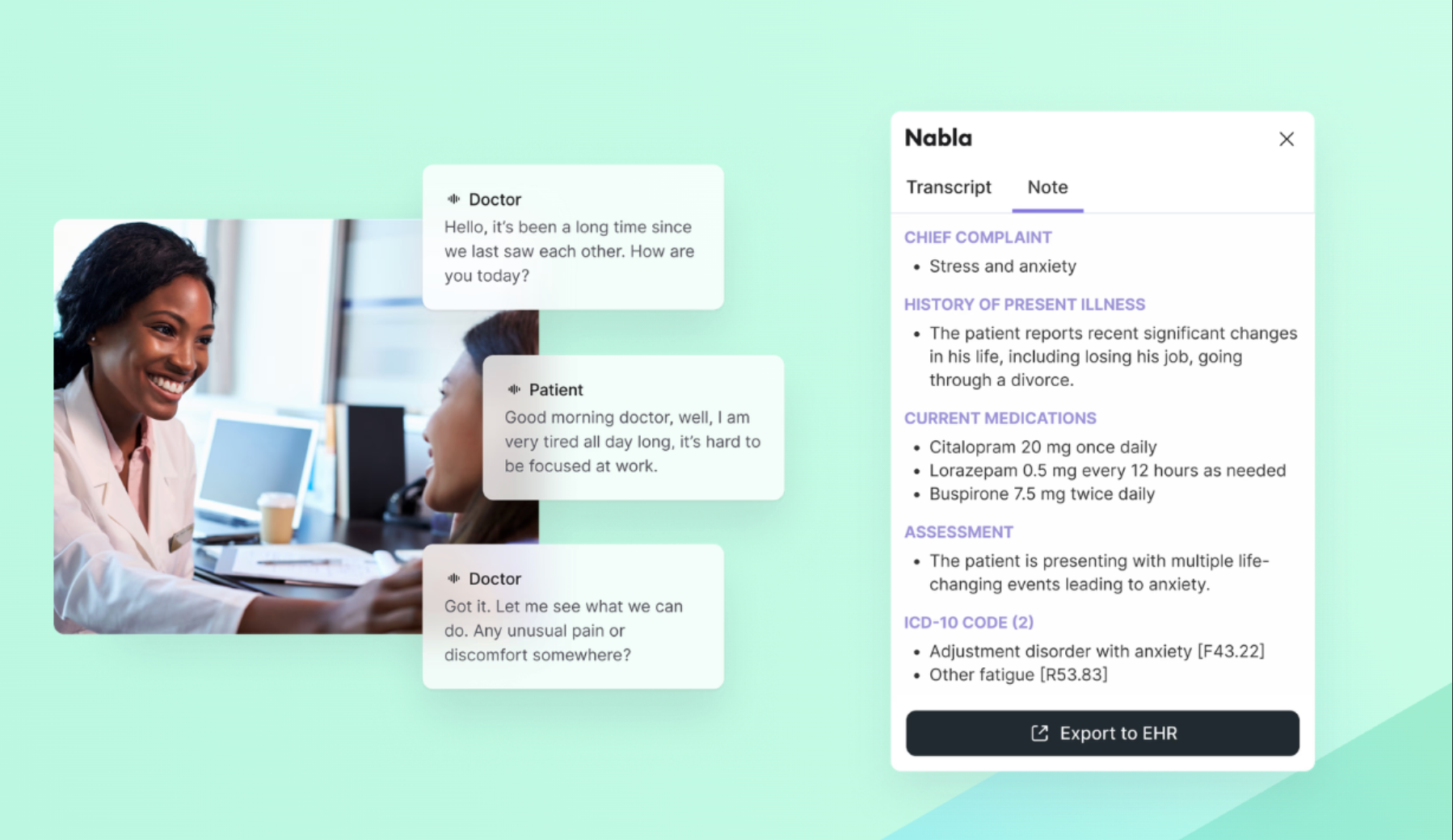
Today, Nabla operates as an AI clinical assistant, combining large language models with a proprietary layer that structures medical data, orchestrates model outputs, and integrates directly into clinical workflows.
In practice, the tool listens to consultations (without storing audio), generates structured clinical notes in real time, drafts letters and summaries, and integrates directly into existing medical record systems.
“This is addressing one of the most persistent friction points in healthcare: the administrative overload that distorts how doctors practise.”
Fixing broken workflows
The deeper issue, Soffiati explained, goes beyond note-taking. Healthcare workflows today are fundamentally inefficient:
- Doctors write notes after consultations, from memory
- Assistants reprocess incomplete information
- Patient records are fragmented
- Instructions are unclear
The result is friction, everywhere. “Everyone is rushing. The pressure is huge, particularly in hospitals. It’s not a good experience for doctors or patients,” she said.
This inefficiency comes at a cost. Poor documentation, duplicated tasks, and unclear care pathways can lead to redundant treatments, delayed diagnoses, and avoidable expenses for the healthcare system.
By structuring data properly and in real time, Soffiati argues that AI assistants like Nabla can improve care accuracy, reduce duplication, and streamline decision-making. When asked whether such tools might replace medical assistants, she is quick to push back.
“Many medical assistants didn’t want to be secretaries," she said. "They wanted to help care for patients.”
The goal, she explains, is not substitution but rebalancing by shifting staff away from clerical work and back toward patient-facing roles.

Cracking the French market
Despite the French DNA, one of the surprising twists to Nabla's success to date is that it has come primarily outside its home country.
Nabla has already scaled to 100,000 practitioners, with the bulk in the US. France is a different story. It's more regulated, more fragmented, and slower to adopt.
In that regard, Nabla is betting that having a former insider on its team will be an advantage.
"She will lead the development of Nabla in France and its partnerships with a simple and concrete objective: to free caregivers from their administrative tasks to give them back medical time," the company said in its announcement. "This extraordinary career has given her a detailed understanding of the French health system and the challenges of all its players. She now brings to Nabla an approach that is both structured and operational, forged by a solid experience in health innovation and European digital regulation. After our success in the United States, the acceleration in France opens a new development phase for Nabla."
Soffiati believes France is ready to embrace this transformation. AI assistants are spreading faster than previous digital tools like electronic health records, which took nearly 20 years to become widespread and are still unpopular among doctors.
Nabla has already struck partnerships with Centre hospitalier d'Arles, Greater Paris University Hospitals - AP-HP, Institut Arthur Vernes, and Centre Hospitalier d'Avignon.
The key, she pointed out, is simplicity. “We need to fit into workflows, not create more add-on tools,” she said. “France has many competitors, which forces a good product-market fit."
The limits of LLMs in healthcare
Despite her enthusiasm, Soffiati is clear about the technology itself.
“We’ve reached the ceiling of what LLMs can do in healthcare,” she said.
The issue isn’t just performance. Its reliability and explainability. “We still can’t understand why the model works and then suddenly sometimes won’t,” she said.
Even with strong safeguards and continuous testing, hallucinations remain a structural limitation of LLMs. Today, Nabla reaches around 95% accuracy. High, but not enough in a clinical setting.
“LLMs are designed to produce an answer, no matter what. Sometimes that answer is incorrect. Obviously, in healthcare, that’s not good enough,” Soffiati said.
Enter AMI Labs and the “post-LLM” future

This is where things get particularly interesting.
Nabla’s trajectory is now bound to AMI (Advanced Machine Intelligence) Labs, the research lab co-founded by Yann LeCun. Whilst continuing to work at Nabla, Lebrun also joined AMI part time as CEO. Lebrun and LeCun's connections stretched back years, and the latter had served as an advisor to Nabla.
Meanwhile, day-to-day operations at Nabla continue under co-founder Delphine Groll, as the company searches for a new CEO to guide its next stage of growth.
Still, the move raised some eyebrows, coming so soon after the latest funding round and the apparent momentum behind Nabla. The two companies are backed by some of the same investors, including Cathay Innovation and HV Capital.
As part of the leadership change, Nabla signed an exclusive partnership with AMI, giving it early access to emerging AI technologies. Taken together, the moves signal a coordinated push to align cutting-edge AI research with real-world clinical deployment, potentially positioning Nabla at the forefront of agentic healthcare AI.
In this case, that means leveraging breakthroughs AMI hopes to make in "world models," a new class of AI systems designed to overcome the limitations of today’s LLMs by enabling more reliable, deterministic, and simulation-based reasoning.
Unlike LLMs, which predict text, these systems aim to reason about real-world situations, integrate structured data, behave more deterministically, and adapt to specific environments, such as healthcare.
The bet is to combine LLMs with world models to unlock truly autonomous, regulator-ready AI systems in healthcare. This would allow Nable to move from a documentation assistant to a full clinical support system that will assist doctors with diagnosis, decision-making, and treatment plans.
“We need a new model,” Soffiati said. “LLMs were a great and necessary first step, but they can’t solve everything...These new World model AI systems will help doctors make better decisions, but not replace them.”
A system-level ambition
For Soffiati, the goal is not just Nabla's growth. It’s systemic impact.
Burnout, administrative overload, and loss of meaning are no longer marginal issues: they are structural. AI, in her view, offers a rare opportunity to tackle them simultaneously.
“We can’t save the French healthcare system without clinicians,” she said. “My goal is to help doctors reconnect with the core of their role: clinical judgment, patient interaction, and continuity of care.”
If Nabla's plan to expand its capabilities works, the impact goes beyond productivity: better patient follow-up, more relevant treatments, fewer unnecessary procedures, ultimately meaning lower structural costs for the healthcare system.
Soffiati is under no illusion about the scale of that challenge.
“We’re only at the beginning," she said. "The real shift will come when AI can reason, not just generate.”







